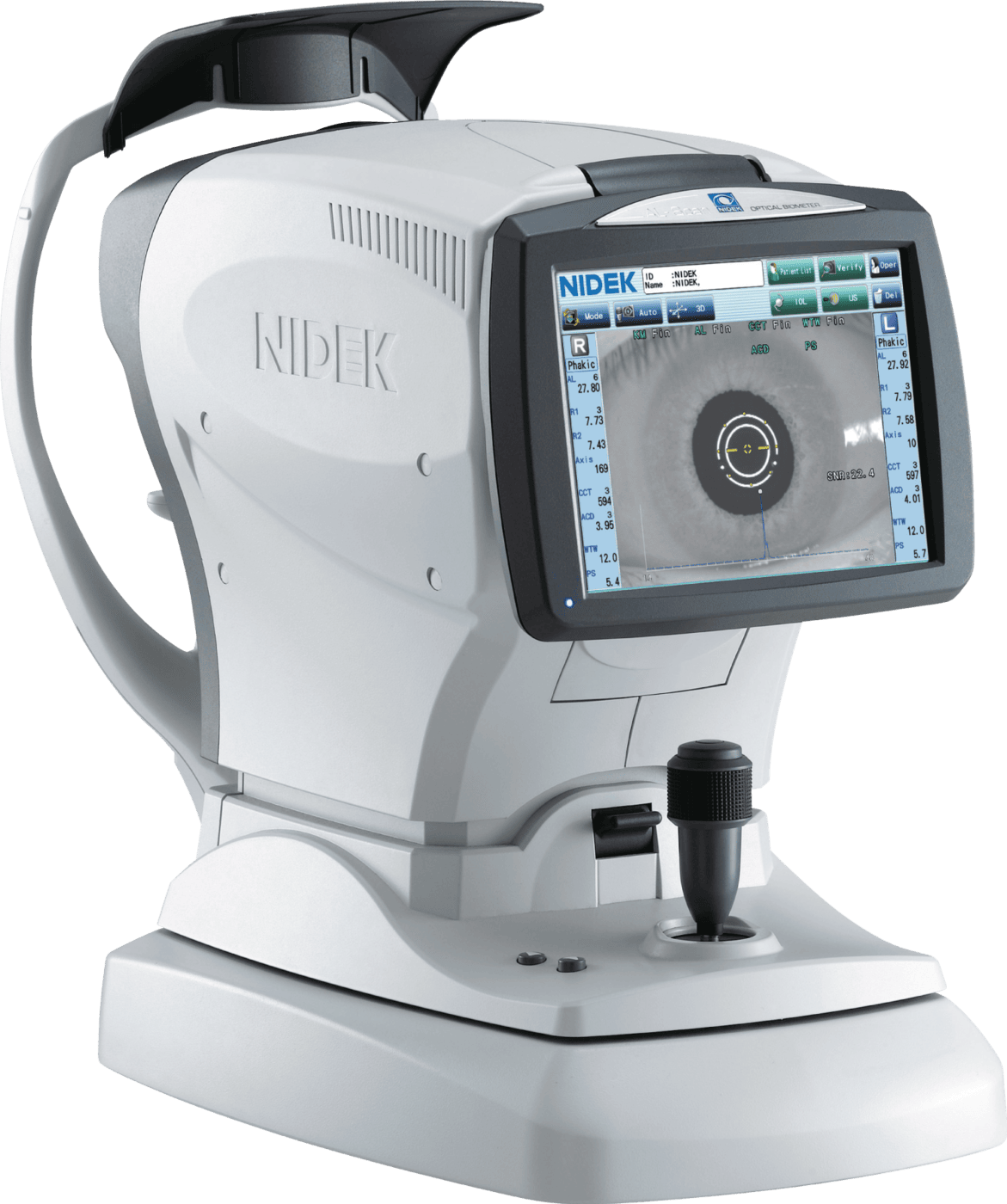
Accuracy, reproducibility, and ease of use are hallmarks of the NIDEK AL-Scan optical biometer
In refractive cataract surgery, a fraction of a diopter or a few degrees of astigmatism one way or the other can mean the difference between delight and disappointment for patients, even when the surgery was otherwise textbook perfect.
Our two-surgeon practice in Niskayuna, NY, is known as one of the premium cataract surgery practices in the region. About 80% of our patients choose some sort of astigmatism-correcting or presbyopia-correcting technology.
While the patient’s experience in our practice contributes to our high conversion rate, so does the quality of our measurements. Although it may sound like a cliché, a surgeon is really only as good as his or her tools, whether intraoperatively or preoperatively. Accuracy, reproducibility, and ease of use are high on the list of must-haves when planning our cataract surgeries.
ADDRESSING USER VARIABILITY
In our practice, our two experienced technicians were performing biometry with the IOLMaster (Carl Zeiss Meditec); however, we noticed there could be significant variability in their readings, sometimes as much as a half diopter or 12 degrees of astigmatic axis, about 10% to 15% of the time. This was frustrating for us and inconvenient for patients, because it required that our clinical research coordinator step in and repeat those measurements.
We are familiar with Nidek technology, as we use the Nidek OPD in our practice, and we felt that the fully automated AL-Scan biometer might have the potential to improve reproducibility and reduce inter-observer variability. We approached the company about performing a study, and they agreed.
ABOUT THE NIDEK AL-SCAN BIOMETER
The Nidek AL-Scan biometer measures six values in 10 seconds automatically, enhancing clinical efficiency. It is equipped with Nidek’s 3D automatic pupil-tracking software, which tracks eye movements on the x, y, and z planes. When the correct alignment is achieved, it immediately captures the image and data, using a function called auto shot, which minimizes the potential for user variability.
The AL-Scan also has a toric-assist feature that draws a line through a prominent vessel or other landmark to indicate the angle from the steepest meridian. The lines and angle are clearly denoted and overlaid on the eye image to assist with toric IOL alignment during surgery.
The AL-Scan intuitively assists technicians as they position patients for biometry. If a patient’s chin is too low or if the machine is too far away, for example, it alerts the technician and describes the needed adjustments. The AL-Scan is like a self-driving car and has a minimal learning curve.
COMPARING INTER-OBSERVER VARIABILITY
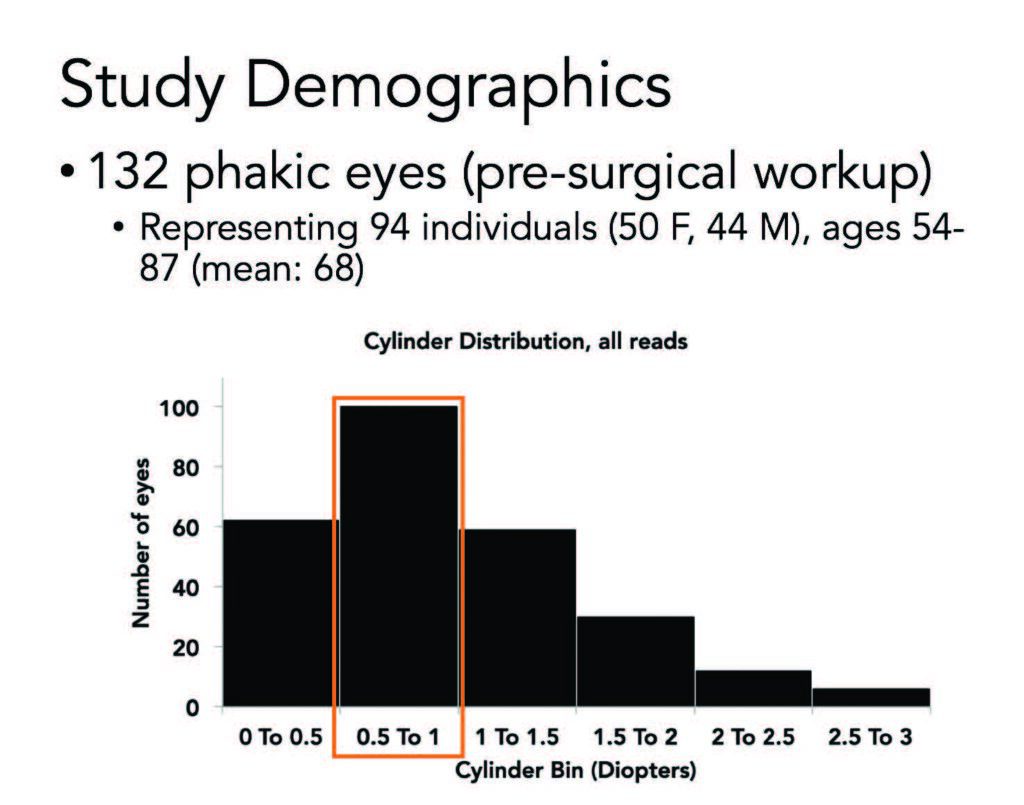
Our study was designed to evaluate inter-observer variability between the fully automated (Nidek AL-Scan) and the semi-automated (IOLMaster) biometer1. The goal was to assess test/retest variability in the clinic. This was strictly a reproducibility study, and we were most interested in keratometry readings, because astigmatism correction is the upgrade most often chosen by our patients.
We evaluated scans of 132 phakic eyes of 94 individuals between the ages of 54 and 87 years (Figure 1). Two scans were taken on each instrument, one by each technician, for a total of four scans per eye. We compared measurements of axial length, anterior chamber depth, and white-to-white distance, and performed vector analysis for cylinder.
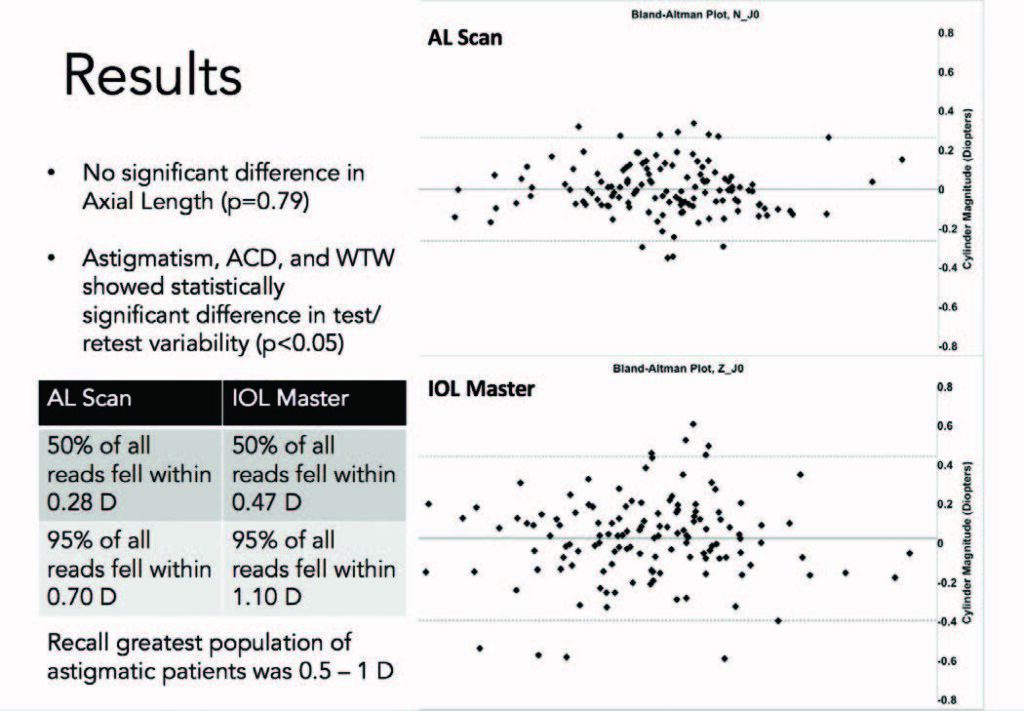
After analyzing the data, we found significantly less test/retest variability with the AL-Scan versus the IOLMaster. Specifically, we found statistically significant differences in measurements of astigmatism, anterior chamber depth, and white-to-white distance (Figure 2). We found no statistically significant differences in axial length measurements.
ACCURACY AND REPRODUCIBILITY
The value of reproducible biometry readings cannot be overemphasized. Not only do patients who are seeking cataract surgery have high expectations for their refractive outcomes, but they often present challenges in addition to cataracts. Many have had LASIK, PRK, or RK, and some have droopy eyelids or dry eyes, all of which can skew preoperative readings.
We were all greatly impressed by the accuracy of the data we obtained from the AL-Scan during our study, but taking a closer look at the technology, it made sense. The AL-Scan uses two mire rings, each providing 360 measurements for a total of 720 data points, compared with the six data points measured by the IOLMaster.
The accuracy and consistency of keratometry readings are very important when our surgeons are planning astigmatic corrections, either surgically, using femtosecond limbal relaxing incisions, or with toric lenses. Our tolerance is less than 5 degrees at 1.00 D between four different sets of keratometry measurements (IOLMaster, Oculus Pentacam, Nidek OPD, and Nidek AL-Scan). Each degree is critical. With consistent, accurate readings, our surgeons can be confident that their outcomes will be on target.
When dealing with post refractive surgery patients, we frequently use intraoperative aberrometry, and we really enjoy seeing the aberrometry data match up perfectly with our preoperative measurement data. It assures us that we were correct in our assessment from the beginning. We dislike last-minute surprises as any surgeon would.
ENHANCED EXPERIENCE FOR PATIENTS
Patients appreciate the speed of the tests performed by the Nidek AL-Scan biometer, particularly if they have difficulty maintaining position because of a physical impairment, such as a neck or spine problem, or if they are unable to follow directions.
Our ability to obtain accurate readings the first time factors into the overall positive experience for patients. Our mantra is, “Do it once. Do it right.” Our technicians love the AL-Scan, because it is fast and user-friendly.
INSPIRING CONFIDENCE
We have been using the Nidek AL-Scan biometer since 2016, and we use it on all of our cataract patients, regardless of whether or not they choose a premium procedure.
Having reproducible keratometry readings and reliable measurements is critical, not only for planning surgery but also for performing cataract evaluations. When a patient is sitting in the chair after having undergone extensive testing, our surgeons can quickly review the data and recommend what they feel is the best option for that patient. They can confidently rule in or rule out certain lenses or procedures for specific patients because they trust they have the most accurate readings possible with the Nidek AL-Scan biometer.
Lemanski B, Lemanski N, Cheng M. Observation of Inter-Observer Variability Between an Automatic Biometer (Nidek AL-Scan) and a Semi-Automatic Biometer (Zeiss IOLMaster). Paper presented at: Annual Meeting of the American Society of Cataract and Refractive Surgery; May 5-9, 2017; Los Angeles, CA.
CONTRIBUTORS
Brian Lemanski
∙ Clinical Research Coordinator, private practice of Mabel M.P. Cheng, MD, and Nicole Lemanski, MD, Niskayuna, NY
∙ [email protected]
∙ Financial disclosure: None
Mabel M.P. Cheng, MD
∙ Private practice, Niskayuna, New York
∙ Financial disclosure: None
Nicole Lemanski, MD
∙ Private practice, Niskayuna, New York
∙ [email protected]
∙ Financial disclosure: None
For more info about the NIDEK AL-Scan optical biometer, visit: https://usa.nidek.com/al-scan